
 The medical condition that is known as cracked heels can develop for a variety of reasons. These can include walking barefoot, standing for extended periods of time throughout the day, or from wearing shoes that have an open back. Additionally, there are medical causes that may significantly contribute to the onset of cracked heels. These can consist of vitamin deficiencies, thyroid disorder, and psoriasis. The symptoms that are often associated with this ailment are pain, red skin, itchiness and inflammation. If you have developed cracked heels, it is suggested that you confer with a podiatrist who can recommend treatment techniques.
The medical condition that is known as cracked heels can develop for a variety of reasons. These can include walking barefoot, standing for extended periods of time throughout the day, or from wearing shoes that have an open back. Additionally, there are medical causes that may significantly contribute to the onset of cracked heels. These can consist of vitamin deficiencies, thyroid disorder, and psoriasis. The symptoms that are often associated with this ailment are pain, red skin, itchiness and inflammation. If you have developed cracked heels, it is suggested that you confer with a podiatrist who can recommend treatment techniques.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact the podiatrists from The Foot & Ankle Center of New Jersey. Our doctors can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact our office located in Paramus, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Cracked heels may make you want to think twice about showing off your feet in warmer weather. However, cracked heels may be harmful to more than just the appearance of your feet. If deep fissures and cracks develop in your heels, they may make walking and standing painful for you. Additionally, these openings make way for germs to enter through your skin and cause infection.
There are several different causes of cracked heels. One of the most common reasons for this ailment is dry skin. This problem may make your keeps feel rough tight and itchy. Dry skin may be caused by cold air, extremely hot water, harsh soaps, and aging. Skin disorders such as eczema and psoriasis may eventually lead to dry skin. In some cases, complications may arise from cracked heels. Some of these complications are a loss of feeling in the heel, cellulitis, or a diabetic foot ulcer.
There are ways you can try to prevent getting cracked heels. One of the best ways to do so is to avoid wearing flip flops and sandals because these shoes increase your risk of drying out your feet. You should also avoid wearing shoes with a tall skinny heel, because these shoes cause your heel to expand sideways. At night, you should slather on a thick moisturizing cream on your feet and then cover them in socks to keep your feet moisturized overnight. Drinking water to stay hydrated is also a good way to ensure that your skin doesn’t become dry.
If you suffer from a severe case of cracked feet, you should make an appointment with your podiatrist to see what treatment methods are best for you.
 The metatarsal bones are the foot bones that connect the toes to the ankles, and stress fractures occur as small breaks in the bones due to repeated stress. Those who have increased their activity level, put pressure on the feet, or have a bone condition are at a higher risk for developing a stress fracture. Generally, the pain from a metatarsal stress fracture starts over a wide area of the foot during activity, but goes away with rest. Left untreated, the pain will be present all of the time. If you are experiencing this kind of pain, it is important to consult with a podiatrist. X-rays or a bone scan may be needed to make a proper diagnosis, and orthotics or a cast may be necessary. A podiatrist will also be able to help determine when it is safe to go back to physical activity.
The metatarsal bones are the foot bones that connect the toes to the ankles, and stress fractures occur as small breaks in the bones due to repeated stress. Those who have increased their activity level, put pressure on the feet, or have a bone condition are at a higher risk for developing a stress fracture. Generally, the pain from a metatarsal stress fracture starts over a wide area of the foot during activity, but goes away with rest. Left untreated, the pain will be present all of the time. If you are experiencing this kind of pain, it is important to consult with a podiatrist. X-rays or a bone scan may be needed to make a proper diagnosis, and orthotics or a cast may be necessary. A podiatrist will also be able to help determine when it is safe to go back to physical activity.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact the podiatrists from The Foot & Ankle Center of New Jersey. Our doctors can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our office located in Paramus, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.
 The tibial nerve is located in a small tunnel surrounded by tendons in the inner side of the ankle. Tarsal tunnel syndrome can develop when this specific nerve becomes compressed, and is often accompanied by pain and swelling. It may happen as a result of enduring an ankle injury, such as a sprain or fracture, or from having bone spurs. Mild relief may be found when the affected foot is elevated, and it may help to take anti-inflammatory medication. In severe cases, surgery can be a viable option to permanently reduce or eliminate the pain that is associated with this condition. If you have developed this ailment, it is strongly recommended that you speak with a podiatrist who can help you choose the correct treatment option.
The tibial nerve is located in a small tunnel surrounded by tendons in the inner side of the ankle. Tarsal tunnel syndrome can develop when this specific nerve becomes compressed, and is often accompanied by pain and swelling. It may happen as a result of enduring an ankle injury, such as a sprain or fracture, or from having bone spurs. Mild relief may be found when the affected foot is elevated, and it may help to take anti-inflammatory medication. In severe cases, surgery can be a viable option to permanently reduce or eliminate the pain that is associated with this condition. If you have developed this ailment, it is strongly recommended that you speak with a podiatrist who can help you choose the correct treatment option.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact the podiatrists of The Foot & Ankle Center of New Jersey. Our doctors can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
The Effects of Tarsal Tunnel Syndrome
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact our office located in Paramus, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Tarsal tunnel syndrome is a condition in which there is a compression of the posterior tibial nerve. The posterior tibial nerve runs along the inside of the ankle into the foot. Tarsal tunnel syndrome is named for the tarsal tunnel, which is a thin space along the inside of the ankle beside the ankle bones. This space contains various nerves, arteries, and tendons, and includes the posterior tibial nerve. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome the tibial nerve is compressed, causing tingling or burning, numbness, and pain.
Common causes of tarsal tunnel syndrome involve pressure or an injury. Injuries that produce inflammation and swelling in or around the tunnel may place pressure on the posterior tibial nerve. Direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or trauma to the tibial nerve, can result in tarsal tunnel syndrome. Diseases that damage nerves, such as diabetes or arthritis, may cause tarsal tunnel syndrome. Those with flat feet are at risk for developing the condition, as the extra pressure and strain placed on the foot may compress the posterior tibial nerve.
Feeling different sensations in the foot at different times is a common symptom of tarsal tunnel syndrome. An afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg. Symptoms are primarily felt on bottom of the foot and/or the inside of the ankle. Symptoms can appear suddenly and may occur due to overuse of the foot.
To diagnose tarsal tunnel syndrome, your podiatrist may examine the foot and tap the posterior tibial nerve to see if symptoms surface. He or she may also order an MRI to determine if a mass is present.
Treating tarsal tunnel syndrome will depend on the decision of your podiatrist. Multiple options are available, however, and can include rest, ice, immobilization, oral medications such as anti-inflammatory drugs (NSAIDS), physical therapy, injection therapy, orthotics, supportive shoes, braces, and surgery.
A bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.
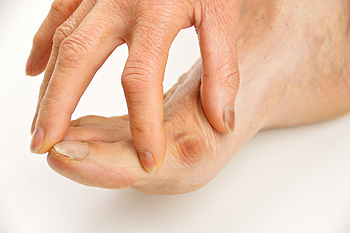 A bony bump that extends around the base of the big toe joint may be referred to as a bunion. It can be difficult to wear shoes that fit properly as it grows, and this may cause pain and discomfort. Additional symptoms can include redness, swelling, and it may interfere with accomplishing daily activities. Some of the reasons bunions develop may include inherited foot structures such as flat feet, or wearing shoes that do not fit correctly. Additional reasons can include existing medical conditions such as rheumatoid arthritis, and certain nerve conditions can also affect the feet. If the bunion is severe and causes distress throughout the day, surgery may be an option for removal. If you have developed a bunion, it is strongly suggested that you are under the care of a podiatrist who can determine the extent of the deformity and provide effective treatment options.
A bony bump that extends around the base of the big toe joint may be referred to as a bunion. It can be difficult to wear shoes that fit properly as it grows, and this may cause pain and discomfort. Additional symptoms can include redness, swelling, and it may interfere with accomplishing daily activities. Some of the reasons bunions develop may include inherited foot structures such as flat feet, or wearing shoes that do not fit correctly. Additional reasons can include existing medical conditions such as rheumatoid arthritis, and certain nerve conditions can also affect the feet. If the bunion is severe and causes distress throughout the day, surgery may be an option for removal. If you have developed a bunion, it is strongly suggested that you are under the care of a podiatrist who can determine the extent of the deformity and provide effective treatment options.
If you are suffering from bunion pain, contact the podiatrists of The Foot & Ankle Center of New Jersey. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
Symptoms
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact our office located in Paramus, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.